Caregivers need to keep a close eye on elderly patients to avoid pressure ulcers from occurring. Pressure ulcers (also called decubiti, or bedsores) are blisters or breaks in the skin caused when the body’s weight presses blood out of a specific area. Pressure ulcers are commonly found in bedridden patients or people with mobility challenges who do not get up to move frequently enough. According to the National Pressure Ulcer Advisory Panel estimates that 2.5 million American develop pressure ulcers each year.
The most common areas for sores are the bony areas—tail bone, hips, heels, and elbows. Damage can range from a change in color in unbroken skin to deep wounds that extend down to the muscle or even bone. How much time it takes a pressure sore to heal depends on how advanced it is. Prevention is key.
The skin breakdown starts from the inside and works up to the surface. Damage can happen in as little as 15 minutes. For people with fair skin, the skin tone may change to dark purple or red and does not turn pale under fingertip pressure. For people with dark skin, this area may become darker than normal.
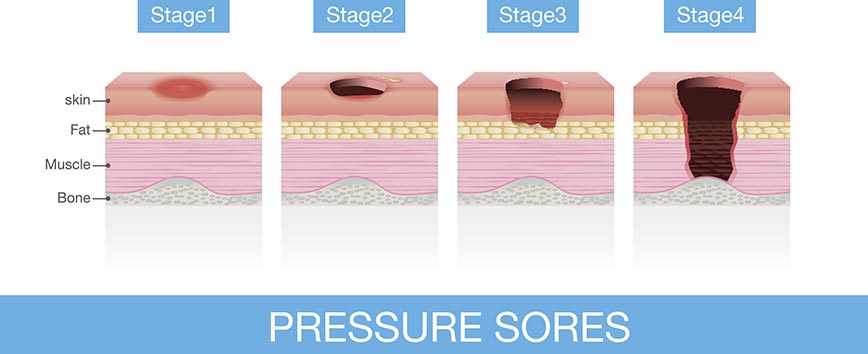
This is one case where an ounce of prevention really is worth a pound of cure. Pressure sores that are not treated can lead to hospitalization and might require skin grafts.
 Check the skin daily. (Bath time is ideal.)
Check the skin daily. (Bath time is ideal.)If you see bedsores in your daily checking of the skin, alert the patient’s healthcare team. The patient will need to be closely observed to ensure the sore is not worsening. Reduce the chance of further infection by wearing disposable gloves when you provide care.
Hope’s Family Caregiver Education Series is available to any member of the community who is currently engaging as a caregiver to a loved one living with a terminal diagnosis or a disabling chronic condition, regardless of whether your loved one is a Hope Hospice patient. The free 12-class series covers a variety of topics and provides training, education, support, and resources relevant to family caregivers. Plus, much like a support group, these classes provide an opportunity to connect with others who have shared experiences.